
Shin splints
The term “shin splints” refers to pain along the shin bone (tibia) — the large bone in the front of your lower leg. Shin splints are common in dancers, military recruits and other athletes whose lower extremities are subjected to repetitive stress.
Medically known as medial tibial stress syndrome, shin splints often occur in athletes, or novice runners who have recently intensified or changed their training routines. The increased activity overworks the muscles, tendons and bone tissue. Early treatment is key to healing shin splints, and to preventing the condition from becoming worse.
What Exactly Are Shin Splints?
Although the term is used almost universally to describe sports-related shin pain, it is clearly not a very scientific name for a medical condition. In fact, “shin splints” is an umbrella term covering more than one type of shin injury.
The most common subcategories of shin splints include:
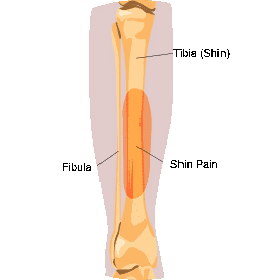
Medial tibial stress syndrome: Caused by inflammation where the anterior tibialis muscle attaches to the tibia, medial tibial stress syndrome accounts for 10 to 15 percent of running injuries, and 60 percent of lower leg pain syndromes.
Compartment syndrome: Chronic compartment syndrome in the shin can develop from swelling or bleeding within a muscle compartment, made up of muscle fibers, capillaries and nerves surrounded by fascia. Because the fascia does not stretch, pressure builds within the compartment, reducing blood flow to the muscle and nerves.

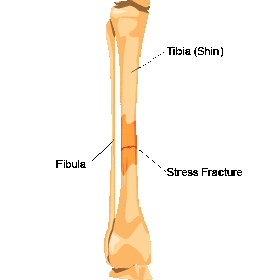
Tibial stress fracture: Fractures of the tibia can occur from repetitive stress, causing pain and inflammation. Stress fractures are often difficult to detect with Xray or MRI.
Causes
Shin splints are fundamentally a repetitive overuse injury, brought on by overtraining and inadequate recovery between training sessions. However, other factors may come into play that increase the risk of shin splints.
- Worn, poorly fitting or unsupportive footwear
- Faulty gait mechanics
- Sudden increases in exercise intensity, duration or frequency
- Training on hard surfaces like concrete
- Training on hills
- Imbalances between the shin and calf muscles
Prevention
To help prevent it:
- Running form analysis.A formal video analysis of your running technique can help identify movement patterns like over-striding that can contribute to shin splints. In many cases, a slight change in your running can help decrease your risk.
- Avoid overdoing.Too much running or other high-impact activity performed for too long at a high intensity can overload the shins.
- Choose the right shoes.If you are a runner, replace your shoes about every 350 to 500 miles.
- Consider shock-absorbing insoles.They might reduce shin splint symptoms and prevent recurrence.
- Lessen the impact.Cross-train with a sport that places less impact on your shins, such as swimming, walking or biking. Remember to start new activities slowly. Increase time and intensity gradually.
- Add strength training to your workout.Exercises to strengthen and stabilize your legs, ankles, hips and core can help prepare your legs to deal with high-impact sports.
Treatment
- ESWT (extracorporeal shock wave therapy) to stimulate tissue repair
- Manual therapy
- Foot and calf strengthening exercises
Shin splints can indicate mechanical errors that may lead to more serious injuries down the road.
